Despite My Progress, I Always Fear My Sarcoidosis Will Worsen

The other day, I was sitting on the couch recuperating from my shower. (Yes, for many people with sarcoidosis, a shower is an Olympic event that requires planning, preparation, and recovery — but that’s a story for another day.)
Anyway, I was on the couch trying to relax when, suddenly, my left hand started to hurt. Each knuckle quickly stiffened. I couldn’t close my hand into a fist, but I couldn’t open it all the way, either. And the pain was intense.
Within seconds, my left knee started hurting just as much, with a sharp pressure that left me feeling like my kneecap was being crushed. It spread up my thigh, shooting pins and needles all the way to my hip. No matter how I shifted in my seat, I couldn’t get into a less painful position. Then my right hand started, just like the left. And I got scared.
I can’t go back to that.
Like many people with sarcoidosis, I’ve gotten used to living with chronic pain. It may vary in location, type, and intensity, but it’s always there. I do my best to manage it with a variety of treatments, but nothing takes it away completely.
Still, that becomes a kind of baseline pain: I know what it is, and I can recognize if a new pain denotes a problem that needs to be addressed. When I fell a few weeks ago, I knew the pain was different and required attention. As it turned out, I’d broken my foot and sprained my ankle. I saw the orthopedist, got my boot and walker, and we’re working on my recovery.
But that hand/knee/thigh/hip/hand pain was different. It was much more severe than the pain I’m used to. It immediately took me back to 2015, and I began to panic.
I can’t go back to that.
In 2015, I was in the worst shape of my life. I hadn’t yet been diagnosed with sarcoidosis, but I’d spent four years with rotating misdiagnoses and treatments that didn’t help. That included four years on steroids, which led to a 100-pound weight gain, Cushing syndrome, and many other side effects.
At the time, I had to weigh the damage being done against the benefits I was receiving, and ultimately, I told my rheumatologist I wanted to stop the steroids. We spent most of the year weaning me off, and all my symptoms just got worse.
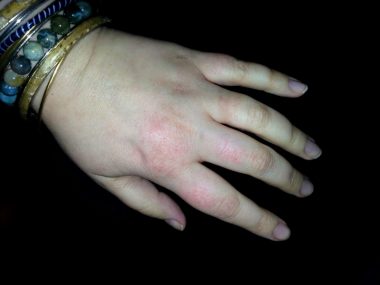
Kerry’s swollen and inflamed hand in 2015. (Courtesy Kerry Wong)
I had severe headaches every day. My neck was stiff and hurting. My skin broke out in painful rashes. My arms, legs, hands, feet, hips, and back were all swollen, stiff, and excruciating. I could barely move, and when I did, I screamed in agony. I couldn’t open a pill bottle or pour myself a drink. I couldn’t stand from a seated position. I couldn’t type on my computer keyboard or even hold my phone.
I was helpless. I felt useless. All I could do day and night was suffer. At 40 years old, I needed my mom to take care of me when my husband went to work. This was not a life I wanted to live.
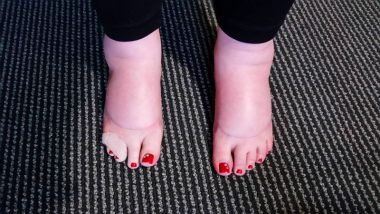
Kerry’s swollen feet and ankles in 2015. (Courtesy Kerry Wong)
Fortunately, my doctor noticed something in my bloodwork during that time, which led me to a pulmonologist for a chest X-ray and a dermatologist for a skin biopsy. After that, I was finally diagnosed with sarcoidosis. I started new treatments and immediately began to improve. I’m still working with my doctors to manage my symptoms, but they are at least manageable now.
Still, there’s always that fear.
I can’t go back to that.
Since I was properly diagnosed and treated, I’ve made a world of progress. The swelling is mostly under control, the rashes are mostly gone, I’m able to move and walk and carry things in my hands without difficulty. For the most part, I’ve gotten to the point where I can live with my sarcoidosis. It may not be the life I’d imagined pre-illness, but it’s beyond what I’d imagined possible in 2015.
Regardless of the progress I’ve made, or perhaps because of it, I always worry about returning to that unbearable state. If my insurance stops covering my medication, I’ll go back to that. If the medication stops working, I’ll go back to that. It can happen for any reason, or no reason at all. That fear lives in the back of my mind, and it can send me spinning or paralyze me with anxiety in an instant.
I can’t go back to that.
I may always live with this fear, but at least now that fear is tempered — outweighed, really — by my gratitude for how far I have come.
***
Note: Sarcoidosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Sarcoidosis News or its parent company, BioNews, and are intended to spark discussion about issues pertaining to sarcoidosis.







Comments
stephen fiege
Hi Kerry, Boy do I know how you feel. Mine is like being on a bad roller coaster ride. Never knowing what the next curve is going to take me. I Have had your swelling problem about 10 years ago. At least doctors couldn't say it was all in my head. They just couldn't tell me what it was at the time. They are still saying you can't blame all your health problems on Sarcoidosis. I tell them you want to bet your wrong on that. Not one doctor would ever bet me on it and I have seen a lot of them. My heart is failing from this disease from just to many years of on and off swelling all over. Good luck and stay well.
🦋 Kerry Wong
Stephen, that was my first thought when my feet/ankles first swelled (and I developed a variety of rashes) too: "at least now they can't say it's all in my head!"
I've had some doctors who blame everything on sarc, and others who don't even acknowledge that new symptoms could be related to it ... either extreme is usually because they don't understand the disease well enough, and don't want to admit that. That's why it's so important (though so hard) to find doctors who are experts in sarcoidosis.
Sending hugs & hope your way!
~🦋
Elizabeth Duruz
Thank you for your article. I am currently in the status of heading back where I was in 2017. My insurance company in all their wisdom is telling me I don't need Remicade.
Remicade is the only medication that has given me my life back and allowed me to feel human again. I have tried Prednisone and Methotrexate with similar experience to yours. It's trading one set of unlivable circumstances (sarcoidosis) for another (medication side effects). Since my diagnosis in 2017, the disease has spread from my lymph nodes and lungs to my bones, skin, and spine. I have no idea how I am going to function if the insurance denies Remicade on my second and final appeal. I feel as though they have just have down a sentence of a slow, painful death to me and there is nothing I can do about it.
I pray others aren't experiencing the same situation.
🦋 Kerry Wong
Oh, Elizabeth, I'm so sorry you're going through this ... and it seems to be happening more and more (see the comment right after yours). This is why we continue to advocate - to share our stories, to learn more from each other. I wish you SO MUCH luck on your appeal.
~🦋
*Another thing to consider is reaching out to the manufacturer. Many pharmaceutical companies have patient assistance programs that can be helpful when the insurance isn't.
Mark Howell
Hi Kerry,
This is such a timely article for me on 2 fronts. First, it took about a year (2019) to be diagnosed with neuro-sarcoidosis. To say that 2019 was a bad year for me is an understatement. I was hospitalized twice, the second time was related to a stroke in the brain stem area caused by the neuro. I'm currently on treatment which includes monthly infusions of Remicade, and weekly shots of methotrexate. Before getting on treatment I suffered some nerve damage in the right side of my brain, an area that manages the left side of my body, so walking is difficult, as the feeling in my left leg, actually the left side of my body up through my midsection is not very good. I mention all of this because I got a letter from Cigna stating that Remicade is no longer a preferred medication and they are offering a "biosimilar" alternative called Inflectra. So I'm a little concerned with this change because there is no data that suggests Inflectra will work for neuro-sarcoidosis, and I can't go back to my 2019 life. My neurologist is in the final stages of appealing. The peer-to-peer was denied, he wrote a letter to Cigna stating medical necessity, but if it is denied I'm not sure what to do. Unfortunately, if the medication doesn't work I'll find out through significant neuro-sarcoidosis symptoms, then what?
Anyone else dealing with this, or currently taking Inflectra for neuro-sarcoidosis?
Thank you,
Mark.
🦋 Kerry Wong
Wow, Mark, that's just so much to deal with. It seems to be happening more and more (see the comment right before yours). It is infuriating to me (aside from scary) when insurance companies make decisions that should only be made between doctor and patient. This is why we continue to advocate - to share our stories, to learn more from each other. I wish you SO MUCH luck on your appeal.
~🦋
*Another thing to consider is reaching out to the manufacturer. Many pharmaceutical companies have patient assistance programs that can be helpful when the insurance isn't.
Christy Haskell
Kerry,
I'm so sorry you had years of suffering before you finally got a diagnosis. It took me 6 months and 4 physicians to finally get diagnosed. My feet swelled just like your and I had hard lumps under the skin on my arms. My primary sent me to a vascular Dr because she was sure it was a vein problem. The last Doctor of the 4, a dermatologist did a biopsy which cam back as sarc. I have been on low dose steroids since but the areas on my arms have never completely gone away. Not sure where I'm going from here!
God bless you,
Christy
🦋 Kerry Wong
Those lumps on your arms sound like what I had on my legs (erythema nodosa). I feel like more and more I'm hearing from people who were ultimately diagnosed by way of skin biopsy, even when we'd been more focused on joints and even lungs. Thank goodness for good dermatologists! Wishing you good days with low-no symptoms!
~🦋
Laurie Kenjar
Hi. I have been on prednisone for five years. Every time I lower my dose my symptoms get worse. I am curious what medications you are using that replaced the steroids. I know everyone's case and treatments are different but I am desperate.
Thank you
🦋 Kerry Wong
Hi Laurie. I definitely know that frustration of feeling like you just can't get off, but staying on isn't so good either. When I was (finally) diagnosed with sarc, I was put on Acthar (corticotropin), along with Methotrexate and Plaquenil. We've had some adjustments since then, and recently added Imuran (azathioprine), a "steroid sparing" immunosuppressant. Too soon for me to tell how well the changes are all working (plus too many things happening at once to really know which to attribute it to). Keep in mind, all of these have pros & cons, and it's important to have a good conversation with your doctor(s). Wishing you luck!
~🦋
Wilma Brown
The feeling of that extreme pain never goes away. Sometimes a a twist or turn brings it all flooding back. Just to remind me how far I’ve come.
🦋 Kerry Wong
What a great way to spin that around, Wilma! Rather than always having the fear, you always have the progress. I love it!
~🦋
Mike de Jong
Hello Kerry
Thanks for all the information how you experienced your Sarcoidose. In 2011 I was diagnosed with pulmonary Sarcoidose, like a lot of patients I started with prednisone, but it only reduce just a little bit. When I started with Remicade for 4 years it improved, even till the point in March 2020 I could stop the treatment. So far so good, I was focused on my lungs just like the pulmonologist, the university of Rotterdam call them self Sarcoidose center. I told him on several consults that I experienced pain in hips and hands. NO reaction, I was thinking perhaps I’m just getting older (57) and did a lot of weightlifting. Just by searching on the internet I found out that Sarcoidose is also very tendo and joints related. The pain in the hips is changing during the last year, it’s moving around. This month I will have an appointment with a rheumatologist and probably start using medication for the hips and shoulders, despite the lungs are doing perfect.
So conclusion: Sarcoidose comes in a lot of different sizes and everybody experience it different, but healthcare for Sarcoidose is still based on your own search and contribution.
Greetings from the Netherlands
Michel
Jennifer
Hi I found a lump under my chin in 2012 . An I was scared to go to the doctor's. Because I didn't know what it was. So I went to the doctor an they sent me to the ent an they biopsy the lump an they found sarcoidosis an they said I was really young you have it. But I'm not sure what type it is but when I get a cold it goes right to my lungs an the doctor has to give me antibiotics an prednisone .
Wendy Schleyer
Yes I took Inflecta and it worked wll till it damaged my liver.
🦋 Kerry Wong
Oh no! So many of these treatments can bring serious risks. It's so important to stay on top of everything and have the docs monitor you closely.
~🦋
DebbraP
Kerry, I can relate to the swelling. I take the diuretic Furosemide for it and it helps -a lot. I also eat "low sodium" and never add salt. You get use to it. Not really but you convince yourself. Once wanted pizza. Never made that mistake again. Bloated up big time. As for the shower, I use a shower chair and even wear my O2 while showering. Use to take me nearly 3 hours to shower/dress, now just one hour. In my old life it only took 30 minutes but hey, I'm living with Pulmonary Sarc and making adjustments. As far as I see it, I'm doing good to be able to bathe and dress myself at all. We all are. I am trying to wean off the Prednisone because I don't know when I can see a doctor again to get a new prescription for it. My husband was my caregiver but recently passed away. I was going to move in with my brother and his family but that's all changed. When I couldn't do any more packing/cleaning for the day, my sister in-law said I was playing victim. Well, I got upset with her so she left and now they say I am not welcome in their home. Never mind that I am sick AND grieving...Lesson learned; pick your battles wisely or you'll be out on your ear.
So yes, all of us Sarkies have our troubles and worries. We plug one hole and another bursts open.
🦋 Kerry Wong
Oh, Debbra, I'm so sorry you're going through that with your sister-in-law. Seems like that can be one thing you could control (where you live), but it sounds like it wouldn't have been a positive environment for you. And to deal with that while grieving and suffering ... I do hope something eases up for you soon.
As for the shower, I'm generally on that 3hr period too - gotta build in all those breaks... even with the chair (though I've only been using the chair again since the broken foot, so that's probably adding to the time, too). Sending hugs & purple power your way!
DebbraP
I hope you can continue with the Remicade, Elizabeth Duruz. A Rheumatologist wanted to try Humira on me, said he was having some success with that. But I never got the chance. Or at least not yet. Maybe in the future. I'm willing.