Sarcoidosis with Cancer Immunotherapy, Mistaken for Cancer Progression
Cancer immunotherapy with Opdivo (nivolumab) and Yervoy (ipilimumab) may or may not trigger sarcoidosis in rare cases, a report from Yale University School of Medicine shows.
The study, “Immune-related sarcoidosis observed in combination ipilimumab and nivolumab therapy,” published in the Journal of the American Academy of Dermatology Case Reports, describes a 60-year-old woman fighting lung adenocarcinoma – a common form of lung cancer. Her cancer had spread to the brain and lymph nodes, and after undergoing surgery for the brain tumor, she started treatment with Opdivo and Yervoy.
Opdivo is a checkpoint inhibitor, a drug blocking a molecule that acts as a brake on the immune system to fight cancer. Yervoy, on the other hand, blocks another factor that allows immune T-cells to become activated to fight cancer.
After two weeks of treatment, the woman developed a rash which the oncologist deemed was a result of the drugs. She was treated with oral diphenhydramine used for allergies, and a corticosteroid cream. The rash resolved and doctors did not stop the immunotherapy.
After two months, physicians noted that the cancer in the lung and lymph nodes had shrunk, but a brain scan indicated that the brain lesion was larger. The immunotherapy was stopped and the woman underwent another brain surgery, which revealed that the lesion was tissue damage caused by radiation therapy.
The woman started the immunotherapy treatment once again. Seven months after starting the treatment, she sought emergency care. She was nauseous, vomiting, confused, and unable to speak.
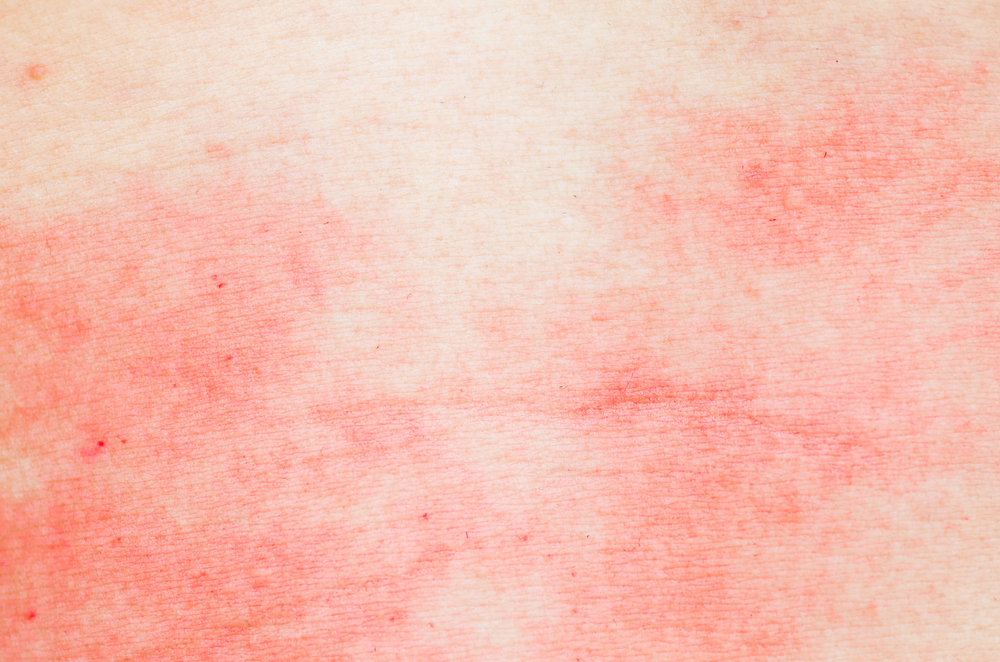
Again, she had a rash on her neck, face, and upper arms. Her lymph nodes in the neck and armpits were normal and her eyes were unaffected. Doctors biopsied the affected skin tissue and concluded that the woman had developed sarcoidosis. The biopsy showed clumps of infiltrating immune cells, called granulomas, which are characteristic of the condition.
Sarcoidosis was limited to the skin and the woman was treated with a corticosteroid cream. Thought the rash improved, it did not disappear. The woman declined further treatment, then died of the cancer three months later.
Researchers emphasize that clinicians should be aware of systemic sarcoidosis because it can easily be mistaken for cancer progression. Only 10 similar cases had been reported previously. The team could not conclude if any drugs contributed to the development of the sarcoidosis and they suggest that more research be conducted to understand if cancer therapies can trigger the disease.






