19 Vials of Blood Made Me Fall in Love With My Doctor
Written by |

The other day, I sent a message to my rheumatologist asking about getting a third shot of the COVID-19 vaccine. It was 11 p.m. on a Sunday, but I had to send it before I forgot. A half-hour later, I received two notifications about a new message and a letter referencing the conditions and medications that make me eligible for a third shot, based on U.S. Centers for Disease Control and Prevention guidelines.
I love her. But this isn’t even what made me fall in love with her.
Most people with chronic illnesses see several doctors before receiving an accurate diagnosis. And when it’s a multisystem disease like sarcoidosis, we’ll also see several specialists after diagnosis, including one for each of the body’s affected systems. In addition to that, sarcoidosis patients usually have a bunch of comorbidities, which prompts the need for even more health professionals.
In all, I see 12 doctors regularly, not to mention those who appear when an unexpected need arises, such as a broken foot.
Improving, but not quite there yet
Starting in 2012, all of the doctors I saw at the time belonged to the same medical group, which offers a range of specialties and providers across several locations in my county. They share a computer network, so all of the doctors in the group can access everyone else’s notes and patient test results, and they’d easily communicate with one another while managing my care.
It was an incredible change from previous years when I would be passed back and forth between gastroenterologists and gynecologists who couldn’t agree on the cause of my abdominal pain or other issues, which left me without answers or relief. The level of communication and shared information I found at the medical group was a godsend.
Over time, though, I realized I had a major problem seeing a dozen doctors in the same medical group: None of them were sarcoidosis specialists. Because they didn’t fully understand my disease, they didn’t know which symptoms were attributed to it.
What that meant, depending on the doctor, was that everything was attributed to sarcoidosis or nothing was. Either way, the doctors were no longer looking for answers because they thought they already had them.
Ultimately, I often ended up doing my own research about my disease, symptoms, and treatments. I’d learn about common complications and comorbidities of sarcoidosis, and see how my symptoms compared.
The search begins anew
Last year, the rheumatologist I’d been with for eight years left her practice unexpectedly without any forwarding information. She was the first doctor I’d seen who looked at more than test results. She really listened to what I said about my symptoms, and didn’t give up when there wasn’t an easy answer. She sent me for a chest X-ray that ultimately led to my sarcoidosis diagnosis.
I needed a new rheumatologist immediately, because at the same time, my insurance company suddenly decided to stop covering the medication I’d been taking for five years. I eventually found a rheumatologist who seemed great — until my insurance wouldn’t cover him.
After a long search, my neurologist finally recommended a rheumatologist she’d worked with before, who she said had a good understanding of my conditions and treatments. I made an appointment, but it was almost four months later. Nevertheless, it was worth the wait.
At my first appointment, the rheumatologist took her time talking to me, and she really listened. She reviewed the medical records I’d sent, examined my joints, and asked if there was anything else I wanted to share. We talked about possible comorbid conditions and potential treatment changes.
Then her medical assistant took 19 vials of blood and a urine sample, and I fell in love.
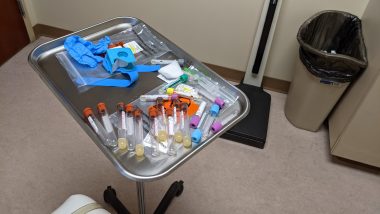
A medical tray with 19 vials and other blood-drawing supplies. (Photo by Kerry Wong)
I’d never had a doctor order so many tests at once. She was thorough. She knew I was a complicated case, and wanted to understand which symptoms were caused by sarcoidosis and which weren’t. More than that, she wanted to figure out the cause of other symptoms and ensure that she was addressing all of my rheumatological needs.
As it turns out, those tests led to two more diagnoses, which explained a lot of what I was experiencing. The answers helped us establish a new treatment plan, which we’re currently working on. At each visit, I fall in love with her even more.
Over the years, I’ve seen a lot of rheumatologists (kissed a lot of frogs?), but I’ve finally found “the one.” And all it took was 19 vials of blood and a urine sample.
***
Note: Sarcoidosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Sarcoidosis News or its parent company, Bionews, and are intended to spark discussion about issues pertaining to sarcoidosis.




Vivian Stoner
Trying to learn more about sarcoidosis and kidney disease.
🦋 Kerry Wong
It's so important to learn as much as we can about these diseases ... and Sarcoidosis News is a great place to start! You can also look to organizations like Foundation for Sarcoidosis Research or specialized sarcoidosis centers like Cleveland Clinic. Good luck!
DebbraP
Congrats, Kerry! Glad you are in good hands and actually like your new Rheumi. I found one that has at least treated three Sarc patients before me. They say most doctors won't even see a single case of it during their career or if they do, it is misdiagnosed. My new Rheumi was about to start me on Humira but life got in the way. But I hope to be able to return to him and begin the treatment. He said he has a female patient about my age (57) with Lung Sarc. He started her on Humira and a few months into it, she was able to get off the Prednisone and oxygen. She still had to stay on Methotrexate but hopefully by the time I return, she will have improved even more. The Rheumatologist also said I probably also have "Sarcoidmyositis", not Polymyositis. I will need lab work for that. But I am hopeful. I have to be. I am homeless living with a very caring and generous family who did not even know me. I was living in a hotel. But they took me into their home without hesitation while I wait for my Widow's Benefits to be approved. And then I plan to get my own little place. I think if I can survive what I have just recently gone through and do it while having Sarcoidosis and on oxygen, I can certainly try the Humira or any treatment that may help. I intend to enjoy life again. Please keep us updated, really hoping you get good news and see improvement.
🦋 Kerry Wong
Wow, Debbra ... it seems like the world has certainly handed you more than your share of challenges ... but also blessings to help you rise through them. Holding on to hope may be difficult at times, but it is the thing that always helps me, too. Thank you for your good wishes, and I will continue to hope for you!
~🦋
GINA WHITACRE
I have been struggling through the search for doctors as well. After being diagnosed in 2015, accidently by a cheat x-ray. I have since had to get a ICD in 2018 due the Sarcoid in the heart causing slow beating, then fast beating. Last month I had a breathing test done by my Sarcoidosis Pulmonary doctor, because I continue to have breathing issues, even though the Sarcoid in the lungs has stopped growing. Now we are looking at Cardiac Pulmonary hypertension, because my heart valve is not resting after it pushes the blood back out. I have had all kinds of of issues with my neck and throat with lymph nodes throughout both recently in the past year. All this while working fulltime in the mental health field around clients who struggle with basic hygiene, before we get into the COVID19 mess. I am struggling at work to get everything done and continue to battle fatigue, due to either the sarcoid or sleep apnea which is severe and untreated due to uncontrollable issues. I am thinking about retirement before I get put into the group homes and have to work face to face with the clients during a 12 hour work shift. I need guidance or a advocate who can walk me through how to retire and explain that sarcoidosis is a multisystem disease and is not cut and dry. I am only working with 2 sarcoid doctors currently and they are not local, everything is mostly by email except for appointments and testing. I was going to take a simple retirement but my supervisor told me with all my issues I should apply for a medical retirement, however the 2 sarcoid doctors I work with do not understand my job and struggles. I am going to retire and move to Florida where I can be seen at the Miami University in the their specialized clinic for sarcoidosis, so I can be seen by doctors specializing in the field 24/7, instead of a few here and a few there but no real research concerning my daily issues with this damn disease. Thank you for your blog and sharing! Can you guild me or provide a location where I could get a advocate to help me with my medical retirement? I have searched websites - concerning sarcoidosis looking for advocates and have been unable to find a link or information about advocates.
If you could help me that would be great - Thank you again for sharing.
🦋 Kerry Wong
Wow, Gina, it sounds like you are really being put through the ringer - it must be so overwhelming. I'm glad you reached out here, as at a minimum you know that you are not alone. As for an advocate who could guide you through retirement/finding the right doctors, etc., I would recommend checking in with the Foundation for Sarcoidosis Research. They have a Patient Navigator program - other sarcoidosis patients specifically trained for exactly that. You can find more info about the program at https://www.stopsarcoidosis.org/patient-navigator-program. Good luck!
~🦋